-
Adopt
-
Veterinary Care
Services
Client Information
- What to Expect – Angell Boston
- Client Rights and Responsibilities
- Payments / Financial Assistance
- Pharmacy
- Client Policies
- Our Doctors
- Grief Support / Counseling
- Directions and Parking
- Helpful “How-to” Pet Care
Online Payments
Referrals
- Referral Forms/Contact
- Direct Connect
- Referring Veterinarian Portal
- Clinical Articles
- Partners in Care Newsletter
CE, Internships & Alumni Info
CE Seminar Schedule
Emergency: Boston
Emergency: Waltham
Poison Control Hotline
-
Programs & Resources
- Careers
-
Donate Now
 By Ashley Lockwood, DVM, DACVECC
By Ashley Lockwood, DVM, DACVECC![]()
angell.org/emergency
emergency@angell.org
617-902-8400
January 2022
Emergency medicine can be both exciting and rewarding. Regardless of size or location, every veterinary hospital has the potential to encounter pet emergencies, from vaccine reactions to anesthetic complications. Often, immediate diagnosis and intervention make the difference between life and death for these pets. So, every veterinary team member needs to broaden their knowledge and sharpen their skills. This is done through good client communication, training, equipment preparation, and understanding the art of triage.
Client Management
Client communication is one of the most important aspects of  emergency preparedness in your practice. Clients remember how they were treated and how you made them feel during a very difficult time. They are faced with life and death decisions and asked to spend hundreds to thousands of dollars in a matter of minutes to hours, with much uncertainty as to the prognosis. These cases need to be handled with empathy while communicating directly and clearly. Veterinarians and support staff need to be properly trained and engaged to ensure that client expectations are clearly understood and managed. Clients need to understand the value of what you have to offer. So, attention to detail, minimizing wait times, and frequent updates are essential.
emergency preparedness in your practice. Clients remember how they were treated and how you made them feel during a very difficult time. They are faced with life and death decisions and asked to spend hundreds to thousands of dollars in a matter of minutes to hours, with much uncertainty as to the prognosis. These cases need to be handled with empathy while communicating directly and clearly. Veterinarians and support staff need to be properly trained and engaged to ensure that client expectations are clearly understood and managed. Clients need to understand the value of what you have to offer. So, attention to detail, minimizing wait times, and frequent updates are essential.
Preparedness
No task is too small or insignificant during an emergency. 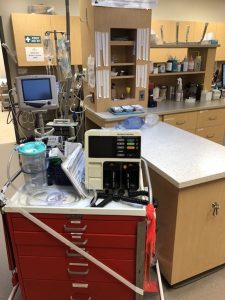 Establishing protocols for emergencies can help to reduce confusion and uncertainty for staff members when handling these cases outside of the daily routine. Having consent and stabilization forms for walk-in emergencies can help expedite diagnostics and therapy before the veterinarian can speak to the owner. Providing support staff with training and scripts can improve the emergency experience on both sides and empowers staff to be calm and confident during a very stressful time. Outlining staff roles during emergencies and continued training will help maintain confidence and teamwork.
Establishing protocols for emergencies can help to reduce confusion and uncertainty for staff members when handling these cases outside of the daily routine. Having consent and stabilization forms for walk-in emergencies can help expedite diagnostics and therapy before the veterinarian can speak to the owner. Providing support staff with training and scripts can improve the emergency experience on both sides and empowers staff to be calm and confident during a very stressful time. Outlining staff roles during emergencies and continued training will help maintain confidence and teamwork.
In addition to training and practice, a well-stocked emergency station and crash cart are required for success. An emergency station that is centrally located (i.e., equidistant from surgery, radiology, laboratory, etc.) or near the entrance and unobstructed is ideal. Additional considerations include:
- Surgical suite level lighting
- Wet table / adjustable scale gurney
- Multiparameter machine with EtCO2
- ER ultrasound
- Suction
- Oxygen with face masks of various sizes and nasal prongs
- Bandage material
- IV catheter materials
- Various fluids and pressure bag
- Crash cart
A crash cart with wheels and at least five to six drawers is recommended. Some crash carts are equipped with portable oxygen as well. Keeping the drawers well labeled and stocked will help with efficiency. A defibrillator and ECG monitor are also suggested and can often fit on top of the crash cart.
| Drawer | Supplies |
| First (top) | Emergency Drugs
– Epinephrine – Atropine – Lidocaine – Calcium gluconate – Dextrose
Assorted syringes with needles attached – Large saline flushes |
| Second / Third | Airway supplies (separated by size)
– Endotracheal tubes – large dogs – Laryngoscopes long blade – Endotracheal tubes – small dogs and cats – Short blade – Stylet – 3cc and 6cc syringes attached to ET tube for cuff inflation – ET tube ties – Tracheostomy tubes |
| Fourth | IV Catheter supplies
– Catheters (multiple sizes) – Tape – Flushes – T-sets |
| Fifth | Centsis supplies
– Large bore catheters – #10 blades – 3-way stop cock – Extension sets – Syringes (12cc-60cc)
Red rubber catheters Cut down packs |
| Sixth | Open-chest CPR packs
Internal defibrillator pattles Blood pressure cuffs EZ IO Gun and catheters |
Triage
Triage is the art of differentiating between stable and critically ill or unstable patients. Every hospital should have established guidelines and trained personnel for telephone and in-hospital triage. Obtaining accurate information from the client is important, but not all clients are equipped with the appropriate knowledge to assess or describe their pet’s condition. Several historical and/or observed problems warrant an immediate evaluation by a veterinarian, including trauma, respiratory distress, active seizures, urethral obstruction, loss of consciousness, excessive bleeding or anemia, poisonings, prolapsed organs, snake bites, heatstroke, open wounds exposing large areas of soft tissue and/or bone, burns, dystocia, or other signs of shock. Failure to appropriately evaluate these patients in a timely manner can quickly lead to death.
Often, the first triage is over the phone or in the front lobby. The front desk or phone staff should have prompts to help determine the urgency of evaluation for each patient. Clients should be questioned about mentation/responsiveness, respiratory effort, gum color, evidence of hemorrhage, or an abnormal limb position. The pet can be further evaluated by a technician or veterinarian based on these answers. While the pet is being evaluated, the client can check in, sign consent forms, and give additional known but brief history using the acronym “AMPLE.”
- A – Allergy to medications or previous blood transfusions
- M – Medications/supplements, dose, last time given
- P – Past pertinent medical history
- L – Last (meal, urination, defecation – were they normal?)
- E – Events (leading to pet presenting, previously administered treatments, response, diagnostics)
The “Primary Survey” is the initial assessment of the emergency patient, and the purpose is to identify life-threatening physiologic problems. This “Primary Survey” follows the ABCs (and Ds) of triage and resuscitation. Whenever a problem is identified, immediate therapy should be initiated.
The ABC(D)s of Triage
- Airway (patent)
- Breathing
- Circulation
- Disability/Dysfunction (CNS)
The airway should be evaluated for foreign objects, mucus, blood, or vomit signs. If fluids (mucus, blood, vomit) are identified, the oral cavity should be suctioned using a large-bore suction catheter. If foreign objects cannot be removed easily, a Heimlich-like maneuver can be performed. If this is not successful, an emergency tracheostomy should be performed without hesitation.
If the patient is breathing, is it dyspneic? Does the patient look like it is going to fatigue or respiratory arrest? If this worsens the patient’s breathing, intubation should be performed immediately, and ventilation should be initiated. In some instances, mild sedation can be helpful to alleviate the stress/anxiety a patient is experiencing.
Obstructive breathing patterns are often slow and deep, while pulmonary contusions, pulmonary edema, pneumothorax, pleural effusions, diaphragmatic hernias, and broken ribs can result in rapid, shallow (restrictive) breathing patterns.
Circulation can be assessed by looking for signs of hemorrhage, fluid loss (externally or into cavities), heart disease, assessing gum color (pale vs. cyanotic vs. brick red), femoral pulse quality, extremity temperature, and/or level of abdominal distention. Vascular access should be obtained rapidly, and fluid or pharmacologic intervention should be determined based on the level/type of shock the patient is exhibiting.
Disability/CNS dysfunction can be evaluated by determining if the patient has a reduced level of consciousness, evidence of seizures (pre-ictal, ictal, post-ictal), abnormal body and/or head posture, abnormal or asymmetric pupil size, and decreased response to light.
While resuscitation and management of the life-threatening problems are occurring, the “Secondary Survey” can begin to identify any other problems related to the trauma or illness. A complete history is obtained, and the entire body is examined (head to tail). Necessary diagnostics samples should be collected. The patient should be set up with a definitive treatment plan, and reassessment is imperative to ensure the patient’s ongoing recovery.