-
Adopt
-
Veterinary Care
Services
Client Information
- What to Expect – Angell Boston
- Client Rights and Responsibilities
- Payments / Financial Assistance
- Pharmacy
- Client Policies
- Our Doctors
- Grief Support / Counseling
- Directions and Parking
- Helpful “How-to” Pet Care
Online Payments
Emergency: Boston
Emergency: Waltham
Poison Control Hotline
-
Programs & Resources
- Careers
-
Donate Now
 By Michael Pavletic, DVM, DACVS
By Michael Pavletic, DVM, DACVS
angell.org/surgery
surgery@angell.org
617-541-5048
Overview
Veterinarians rely on healing by 2nd intention (contraction and epithelialization) for a number of challenging wounds involving most body regions. Myofibroblasts are responsible for wound contraction or the centripetal advancement of the bordering skin. Epithelial cell migration in full-thickness skin wounds originates from the germinal epithelial layer (stratum basale) of the skin edges comprising the perimeter of the defect.
Wound contraction and epithelial cell migration occur independent of each other. Both processes are influenced by the cytokines (growth factors) released in the wound healing process, as well as the microenvironment created by the topical medication/dressing applied to the wound. Young dogs and cats, less than 6 months of age, can heal remarkably well by 2nd intention, primarily as a result of wound contraction alone.
It is important to note that most open wounds that heal by 2nd intention close primarily by wound contraction. From a cosmetic standpoint, this centripetal advancement of healthy skin covers the wound with normal hair-bearing skin. Cosmetically, wound areas that heal by epithelialization are largely devoid of hair follicles and are highly visible in fur-bearing animals, unless adjacent hair regrowth obscures their presence. Additionally, the epithelial layer is only a few cell layers thick and may lack the durability to sustain day-to-day normal “wear and tear.” With unstable scars, surgical resection and closure by skin stretching, skin advancement, skin flaps or free grafts would be necessary.
It must be noted that wound contraction normally peaks out by 42 days after its initiation. When wound contraction effectively ceases, any remaining open wound would require coverage by epithelialization. If a sizeable defect remains at this 6-week juncture of open wound management, the veterinarian must decide whether surgical closure would be the best option for the patient versus prolonged wound care to promote epithelial cell migration.
Wound Closure Considerations
When dealing with contaminated and infected wounds, a variable amount of open wound care is necessary to promote formation of a healthy granulation bed before considering potential wound closure options. Necrotic tissue, contaminants and the resident bacterial population must be addressed with surgical and medical management. During this first week of open wound care, the veterinarian has time to assess the wound daily and formulate a plan on how best to close the wound. Healthy granulation tissue formation is a clear signal to the clinician that healing is underway and the underlying tissues are healthy enough to promote its development. Moreover, healthy granulation tissue forms a protective barrier to help blunt invasive infection. It is important to remember that, after acute injury, tissue swelling with elastic retraction of the traumatized skin margins actually exaggerates the wound size by 25-30% during the first week of trauma. As swelling recedes, typically after the first week of care, the veterinarian can more accurately assess the size of the wound.
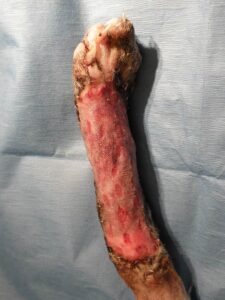
Clinical experience is invaluable for determining whether a given challenging wound can heal by 2nd intention. The size and location of the open wound play a major role in determining whether contraction and epithelialization is a practical and realistic option to close a problematic skin defect. In general, moderate-sized wounds involving the trunk, and smaller problematic wounds involving the extremities, may be prime candidates for 2nd intention healing. For effective wound contraction, the skin around the perimeter of the wound should have a variable degree of mobility and elasticity. This is especially relevant when dealing with lower-extremity defects. Skin defects approaching 180 degrees of the limb circumference normally require reconstructive surgery in the form of skin grafts or flaps. Wounds that are closer to 90 degrees (or less) of the circumference of the limb have a better chance at healing by 2nd intention (Figures 1 and 2).
- Figure 1A: Half the skin circumference of this cats lower hind limb was lost to trauma. Healing by second intention is unrealistic for this wound.
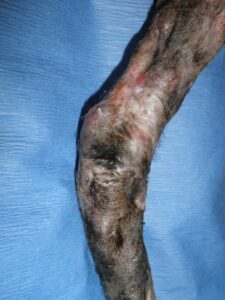
- Figure 2A- Chronic, fibrotic wound bed of several months duration. 2nd intention healing failed to close this wound.
Complications of 2nd Intention Healing
The clinician must be alert to these common factors that delay or prevent wound contraction, including:
- Paucity of loose elastic skin for effective contraction (counter-tension)
- Restrictive scar tissue
- Unhealthy wound bed
- Poor regional circulation
- Repeated regional trauma
- Skin margins failing to attach to the underlying granulation bed* (see Figure 3)
(*The latter point is commonly overlooked by clinicians. A skin margin fully detached from the adjacent granulation bed over time will contract or curl under itself, with epithelial cells migrating over the underlying dermal border. A “pocket wound” forms, preventing normal 2nd intention healing. To promote effective contraction and epithelialization, the contracted skin border may require debridement followed by suturing the skin directly to the granulation bed. Once both surfaces adhere, 2nd intention healing can occur.)
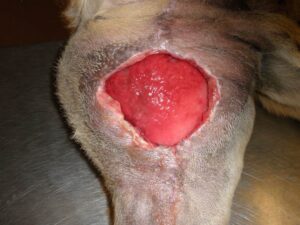
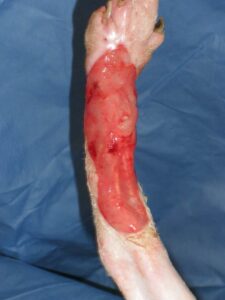
- Figure 3A -Area of surgical dehiscence, inner left thigh of a dog . The skin margins have yet to adhere to the granulation bed, thereby delaying the possibility of healing by second intention.
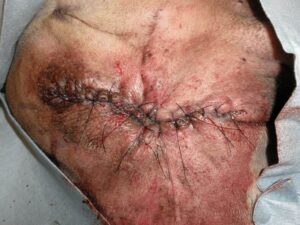
- Figure 3B- Due to the delay in second intention healing and the problematic area of the wound, the skin was mobilized and the wound successfully closed.
Combining 2nd Intention Healing and Reconstructive Surgery
With those wounds that have potential to close by contraction and epithelialization, the veterinarian can opt out to “ride the wave of wound contraction” and see how far the wound can close over the following few weeks (Figure 4). Even if 2nd intention slows and falls short of wound closure, the wound normally is much smaller and surgical closure would be easier and more economical to perform.
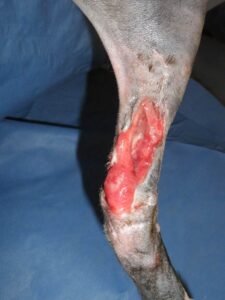
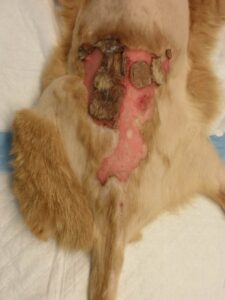
- Figure 4A-Burn eschar, dorsal lumbar area of a cat. This was determined to be a partial and full-thickness burn. Conservative management was initiated, including partial surgical debridement of loose mummified skin followed by topical silver sulfadiazine ointment.
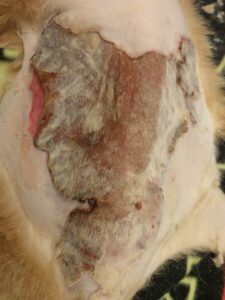
- 4B: Serial debridement and open wound management, week 4. Note the remarkable decrease in the size of this full-thickness wound , secondary to wound contraction. Partial thickness burned areas quickly re-epithelialized from survival of the compound hair.
Lower-extremity defects, secondary to trauma or surgery (e.g., tumor resection), can be closed primarily on a number of occasions with the use of release/relaxing incisions and local skin flaps. In essence, tension-relieving incisions allow closure of a problematic wound while relying on 2nd intention healing to close the incisional (donor) defects created to mobilize the skin. Another option to facilitate closure of a smaller, problematic lower-extremity wound is the use of a small pedicle graft to partially close the defect. A small transposition flap can be developed, not to close the entire wound of the lower extremity, but to close the central portion of the wound. The skin flap essentially closes a major portion of the defect while creating 2 smaller open wounds that can heal more effectively (and faster) by 2nd intention healing.
Final Comments
Advances in reconstructive surgery, including the use of skin flaps, free grafts and skin stretching, enable surgeons to close challenging wounds quickly and effectively. The advantages of primary closure include rapidly returning function to the patient, reducing discomfort associated with prolonged open wound care, and eliminating the cumulative costs and time associated with multiple bandage changes and hospital visits. These advantages are weighed against the costs of surgery and anesthesia. Second intention healing can be an effective option for open wounds, provided that the wound size and location are conducive to this healing process. The veterinarian can always consider surgical closure if contraction and epithelialization slow or fail to close the wound adequately. Combining 2nd intention healing with surgical closure, as noted, also can be a very effective option to consider for challenging wounds.
Mike Pavletic, DVM, DACVS, is the Director of Surgical Services at Angell Animal Medical Center. He is the author of the acclaimed Atlas of Small Animal Wound Management and Reconstructive Surgery, published in 2010 by Wiley Blackwell. For more information about Angell’s Surgery service, please visit angell.org/surgery. To contact Angell’s surgeons by phone or to refer a patient to the Angell Surgery service, please call 617-541-5048 or e-mail surgery@angell.org. You can also reach Dr. Pavletic at mpavletic@angell.org.
Reference:
Pavletic M.M. (2010). Atlas of Small Animal Wound Management and Reconstructive Surgery. Wiley Blackwell, Ames, Iowa.