-
Adopt
-
Veterinary Care
Services
Client Information
- What to Expect – Angell Boston
- Client Rights and Responsibilities
- Payments / Financial Assistance
- Pharmacy
- Client Policies
- Our Doctors
- Grief Support / Counseling
- Directions and Parking
- Helpful “How-to” Pet Care
Online Payments
Emergency: Boston
Emergency: Waltham
Poison Control Hotline
-
Programs & Resources
- Careers
-
Donate Now
 By Patrick Sullivan, DVM, DABVP (Avian practice)
By Patrick Sullivan, DVM, DABVP (Avian practice)
MSPCA-Angell West
avianexotic@angell.org
617-989-1561
Domestic ferrets (Mustela putorius furo) are commonly seen at both primary care veterinary hospitals, as well as avian & exotics specialty practices. Much like dogs and cats, periodontal disease is seen in many ferrets as they age. Similar to those species, ferrets also require routine dental prophylaxis to reduce the risk of permanent damage to the dentition and gingiva. Ferrets have a brachyodont dentition, with 28 to 30 deciduous teeth, and 34 permanent teeth. The dental formula of an adult ferret is 2(I 3/3; C 1/1; P 3/3; M 1/2). Plaque accumulation mineralizes and becomes calculi, which allows an overgrowth of bacteria on the crown and at the edge of the gingiva. The degree of periodontal disease can be categorized into 4 stages, based on the severity of the condition. These stages will be described in greater detail below. When compared to feral ferrets of New Zealand, domestic ferrets have a much higher degree of dental pathology. Diet is thought to play a role in this condition, as both wild and domestic ferrets are obligate carnivores. Dry kibble diets, while nutritionally balanced, can be quite abrasive on the enamel of the teeth. Over time this can cause weakening and discoloration. While semi-moist, or wet foods are thought to promote dental calculi in other species, ferrets have been shown to develop periodontal disease when fed exclusively dry kibble. Whole prey diets may slow the progression of periodontal disease in domestic ferrets, but this may be difficult for some owners. If not made properly, homemade diets are often lacking in essential nutrients.
In addition to periodontal disease, ferrets can also sustain dental trauma. Due to their curious behavior, and penchant for chewing non-food items, fractures of the crowns are not uncommon. The maxillary canine teeth are often damaged due to chewing on cage bars, or other hard objects, or secondary to a fall. Superficial damage to the tooth may also occur, but often times this does not require extraction. Exposure of the pulp cavity, or periapical abscess formation, would warrant extraction of the affected tooth.
Stages of Periodontitis
Stage 1: Gingivitis – Erythema and possible swelling noted at the edge of the gingiva. This condition is caused by bacterial colonization on plaque, which if left untreated, will mineralize and become dental calculi. Calculi will not be able to be removed by brushing, and will require ultrasonic scaling under general anesthesia.
Stage 2: Early Periodontitis – Progression of gingivitis may lead to infection of the gingiva, bone, and surrounding tissue. Gingival recession (up to 25%), or periodontal pocketing, may be noted at this time as well. While not common, abscessation of the gingiva can occur during this stage.
Stage 3: Moderate Periodontitis – Worsening of gingival recession (up to 50%), as well as root exposure are seen in this stage. Large periodontal pockets are identified during probing, and may bleed. Food material may be found in these pockets and between exposed roots.
Stage 4: Advanced Periodontitis – Gingival recession is greater than 50%, often with blood or purulent material around tooth roots. Tooth loss is common at this stage, and extractions of several teeth may be required, despite intervention. Gingiva is often so painful at this point that the patient may need sedation, or even full anesthesia.
Dental Prophylaxis
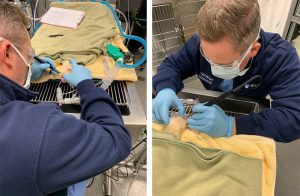
Ferrets requiring a dental prophylaxis will need to be anesthetized and intubated during the procedure. Aside from a physical exam, a preoperative CBC and chemistry panel should be performed to ensure there are no underlying conditions that may increase the anesthetic risk, or change the protocol for the patient. Due to their high metabolic rate, and risk of hypoglycemia, ferrets should only be fasted for 2 hours prior to anesthesia. Much the same as other dental procedures in small animals, once anesthetized, ferrets require endotracheal intubation to protect the airway during ultrasonic scaling and polishing. A cuffed 3.0 endotracheal tube is often used for this, but occasionally this size tube is too large and an uncuffed tube is needed. In this case it is especially important to keep the head angled slightly down, to avoid aspiration. All crowns are scaled using an ultrasonic scaler, and the gingiva is probed for any abnormal pocketing or abscessation. Once it is determined that all teeth appear healthy and no extractions are required, the crowns are polished using an animal safe prophy paste
If extractions are deemed necessary, the technique used will depend on which tooth is being removed. Canine teeth can be removed using a periodontal flap technique, where the gingiva is incised and reflected away, to allow access to the root. A high speed pneumatic drill may be used to burr away surrounding bone, allowing an elevator to be introduced into the socket to break down periodontal ligament attachments. For teeth with multiple roots, it may be necessary to section the tooth into pieces, to allow removal of each root individually. Sockets can then be flushed with a chlorhexidine solution and sutured using polydioxanone suture.
Conclusion
While there is no way to completely avoid dental pathology in ferrets, owners can certainly take proactive steps to try and improve their ferret’s overall oral health. Brushing daily with an animal safe toothpaste and a soft bristled brush is ideal. This is by far the best way to reduce the amount of plaque that accumulates on the crowns and at the edge of the gingiva. Water additives and cat dental treats may be of benefit as well, but all treats must be evaluated for the risk of possible gastrointestinal obstruction if large pieces are bitten off and swallowed whole. Finally, annual, or biannual exams, are needed to be able to evaluate the oral cavity and track any changes in the medical record.
References
- Johnson-Delaney, Cathy A. 2007. Ferret Dental Disorders: Pictorial of Common Clinical Presentations. Exotic DVM 9(2): 40-43.
- Cooper, Janyce. 2017. Ferret Dentistry: No Weaseling About It. Today’s Veterinary Nurse. Jan/Feb.
- Quesenberry, Katherine A., Carpenter, James W. 2012. Ferrets, Rabbits, and Rodents Clinical Medicine and Surgery. Third Edition. St. Louis (MO): Elsevier. Chapter 3, Gastrointestinal Diseases; p. 27