-
Adopt
-
Veterinary Care
Services
Client Information
- What to Expect – Angell Boston
- Client Rights and Responsibilities
- Payments / Financial Assistance
- Pharmacy
- Client Policies
- Our Doctors
- Grief Support / Counseling
- Directions and Parking
- Helpful “How-to” Pet Care
Online Payments
Emergency: Boston
Emergency: Waltham
Poison Control Hotline
-
Programs & Resources
- Careers
-
Donate Now
 By Megan Cray, VMD, DACVS-SA
By Megan Cray, VMD, DACVS-SA
![]() angell.org/oncology
angell.org/oncology
oncology@angell.org
617-541-5136
September 2023
x
x
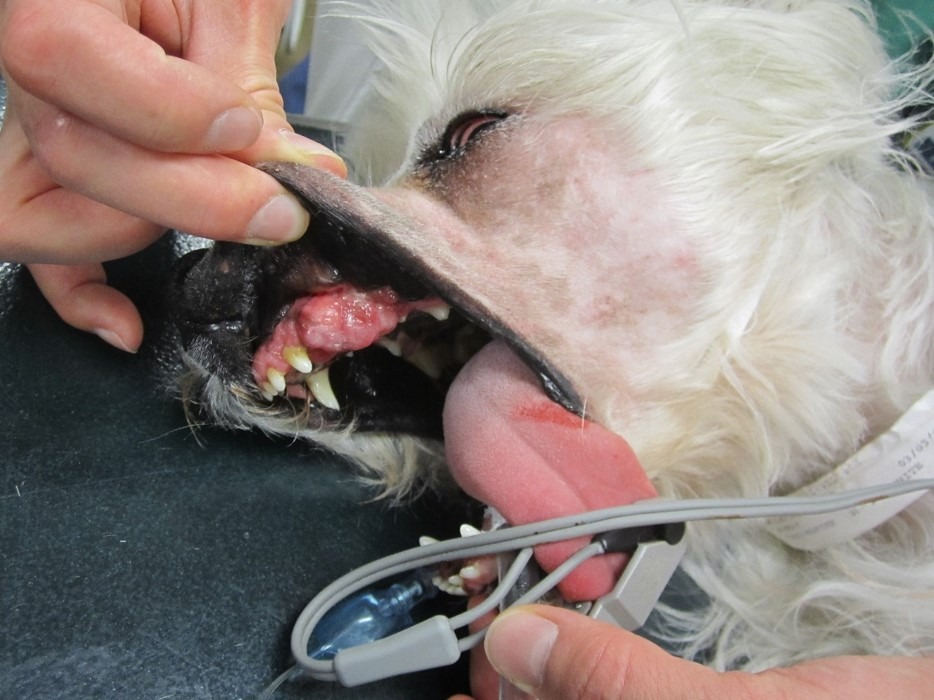
Oral cancer accounts for six to seven percent of canine and three percent of feline cancers. This percentage may increase as veterinary medicine advances and more prophylactic dentals are being performed. Early detection, diagnosis, and treatment can vastly improve the prognosis for canine and feline oral tumors.
Diagnosis and Staging
Many animals present with an oral mass appreciated by their owner. Other possible clinical signs of an oral tumor include increased salivation, epistaxis, weight loss, halitosis, oral discharge, and dysphagia. The tumor diagnosis workup is imperative in determining treatment options and prognosis. The first step is documenting the location and tumor size. Often, an incisional biopsy is needed to obtain a diagnosis. Due to frequent inflammation and necrosis, fine needle aspiration and cytology are often not rewarding. While regional radiographs can detect bone invasion due to imposition, surgeons often elect CT imaging for surgical planning.
The regional lymph nodes of the oral cavity include the mandibular, parotid, and medial retropharyngeal lymph nodes. Any mandibular lymph node enlargement should be documented, and fine needle aspiration should be performed. However, in one study of 100 dogs with oral melanoma, 40% of dogs with normal-sized lymph nodes had metastasis, and 49% of dogs with enlarged lymph nodes did not. Therefore, normal size does not always preclude the presence of metastasis. Chest radiographs or thoracic CT should always be performed in patients with malignant oral tumors to assess for possible metastasis.
Surgical Options
Surgery is the most frequently used modality in the treatment of oral tumors. Mandibulectomies and maxillectomies are generally well tolerated and can provide an excellent outcome. Typically, 2 to 3cm margins are ideal for malignant tumors, while 0.5cm margins are acceptable for benign tumors. While both procedures carry a moderate risk for complications, the majority of these complications are considered minor. Surgical complications that have been associated with these procedures include hemorrhage, aspiration pneumonia, incisional dehiscence, mandibular drift and malocclusion, ranula formation, anorexia, nasal discharge or epistaxis, difficulty prehending, implant migration, oronasal fistula formation, and very rarely death. Most of these procedures do not significantly alter the dog’s or cat’s outward appearance. Owners frequently report high satisfaction following their pet’s surgical procedure.
tumors. Mandibulectomies and maxillectomies are generally well tolerated and can provide an excellent outcome. Typically, 2 to 3cm margins are ideal for malignant tumors, while 0.5cm margins are acceptable for benign tumors. While both procedures carry a moderate risk for complications, the majority of these complications are considered minor. Surgical complications that have been associated with these procedures include hemorrhage, aspiration pneumonia, incisional dehiscence, mandibular drift and malocclusion, ranula formation, anorexia, nasal discharge or epistaxis, difficulty prehending, implant migration, oronasal fistula formation, and very rarely death. Most of these procedures do not significantly alter the dog’s or cat’s outward appearance. Owners frequently report high satisfaction following their pet’s surgical procedure.
Types of Oral Tumors
 The most common oral tumors in dogs are malignant melanoma, squamous cell carcinoma, and fibrosarcoma. Malignant melanoma tends to occur in smaller body weight dogs than other oral tumor types. These tumor types carry a high metastatic rate to the lymph nodes and lungs, holding only a fair to good prognosis following surgery. Non-tonsillar squamous cell carcinoma has a lower metastatic rate (~20%) but depends upon the site. Squamous cell carcinoma contained to the rostral oral cavity generally has a low metastatic rate, and the caudal tongue and tonsil have a high metastatic potential. Following surgery, the prognosis can be good to excellent. Fibrosarcomas most commonly occurs in large-breed dogs. These can be difficult to differentiate from fibromas and, therefore, can be classified as histologically low-grade but biologically high fibrosarcomas. The surgical treatment should be aggressive regardless. If surgically resectable, the prognosis can be good as these are most often locally aggressive, with a metastatic rate to the lymph nodes and chest in <30% of cases.
The most common oral tumors in dogs are malignant melanoma, squamous cell carcinoma, and fibrosarcoma. Malignant melanoma tends to occur in smaller body weight dogs than other oral tumor types. These tumor types carry a high metastatic rate to the lymph nodes and lungs, holding only a fair to good prognosis following surgery. Non-tonsillar squamous cell carcinoma has a lower metastatic rate (~20%) but depends upon the site. Squamous cell carcinoma contained to the rostral oral cavity generally has a low metastatic rate, and the caudal tongue and tonsil have a high metastatic potential. Following surgery, the prognosis can be good to excellent. Fibrosarcomas most commonly occurs in large-breed dogs. These can be difficult to differentiate from fibromas and, therefore, can be classified as histologically low-grade but biologically high fibrosarcomas. The surgical treatment should be aggressive regardless. If surgically resectable, the prognosis can be good as these are most often locally aggressive, with a metastatic rate to the lymph nodes and chest in <30% of cases.
In felines, the most common oral tumor is squamous cell carcinoma. While metastasis is reportedly rare,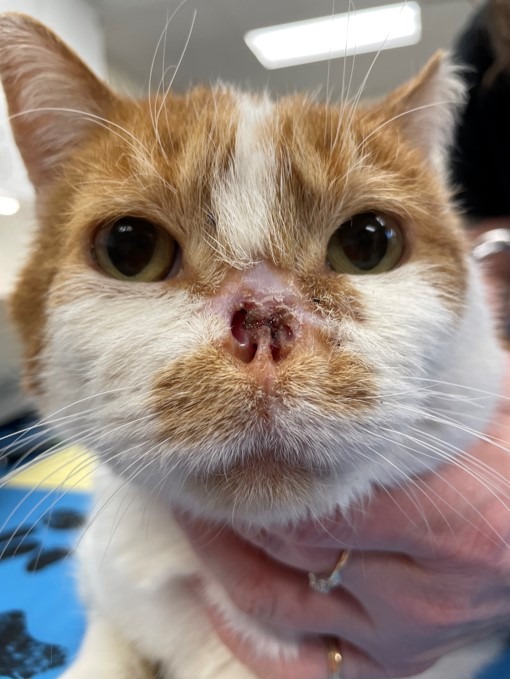 the true incidence is unknown because so few cats have their local disease controlled. Unfortunately, these commonly present without a surgical option and do not respond well to radiation. The prognosis for this tumor type is often poor to fair.
the true incidence is unknown because so few cats have their local disease controlled. Unfortunately, these commonly present without a surgical option and do not respond well to radiation. The prognosis for this tumor type is often poor to fair.
Epulides are benign gingival proliferation arising from the periodontal ligament and can commonly look similar to gingival hyperplasia. These are now subclassified as acanthomatous ameloblastomas and peripheral odontogenic fibromas. While both do not metastasize, these behave slightly differently and are treated differently with surgery. Acanthomatous ameloblastomas are locally aggressive, so a bony margin is needed to remove these tumors. Alternatively, peripheral odontogenic tumors can be cauterized at their base and frequently do not recur.
Tongue masses are rare, with the majority being malignant. The most common type of tongue neoplasia is squamous cell carcinoma. It is important to obtain a biopsy under general anesthesia or heavy sedation. A partial glossectomy can be considered for tumors that are unilateral or rostral. However, many tumors (54%) are midline or bilaterally symmetrical. Radiation is an alternative treatment option for these cases.
Conclusion
Oral tumors are becoming more common in veterinary medicine. The quicker we can work up these cases and obtain a diagnosis, the faster we can start treatment—the earlier the treatment, the better the ultimate prognosis.
x
References
- Berg J: Mandibulectomy and Maxillectomy, in Johnson SA, Tobias KM (eds): Veterinary Surgery Small Animal (ed 2). St Louis, MO, Elsevier; 2018, pp 1663-1677
- Schwartz P. Partial maxillary resection as a treatment for oral-cancer in 61 dogs. J Am Anim Hosp Assoc. 1991;27(6):617-624
- Schwarz P. Mandibular resection as a treatment for oral-cancer in 81 dogs. J Am Anim Hosp Assoc 1991;27(6):601-610
- Zacher Am and Manfra Marretta S: Oral and maxillofacial surgery in dogs and cats. Vet Clin Small Anim 2013;43:609-649
- MacLellan RH, Rawlinson JE, Rao S, et al: Intraoperative and postoperative complications of partial maxillectomy for the treatment of oral tumors in dogs. J Am Vet Med Assoc 2018;252(12):1538-1547
- Bradley RL, MacEwen EG, Loar AS: Mandibular resection for removal of oral tumors in 30 dogs and 6 cats. J Am Vet Med Assoc 1984;184(4):460-463
- Sarowitz BN, Davis GJ, Kim S: Outcome and prognostic factors following curative-intent surgery for oral tumours in dogs: 234 cases (2004 to 2014). J Small Anim Pract 2017;58(3):146-153
- Wallace J, Matthiesen DT, Patnaik AK: Hemimaxillectomy for the treatment of oral tumors in 69 dogs. Vet Surg 1992;21(5):337-341
- Salisbury S: Long-term results of partial mandibulectomy for treatment of oral tumors in 30 dogs. J Am Anim Hosp Assoc 1988;24(3):285-294
- Kosovsky JK, Matthiesen DT, Marretta SM, et al: Results of partial mandibulectomy for the treatment of oral tumors in 142 dogs. Vet Surg 1991;20(6):397-401
- Hutson CA, Willauer CC, Walder EJ, et al: Treatment of mandibular squamous cell carcinoma in cats by use of mandibulectomy and radiotherapy: seven cases (1987-1989). J Am Vet Med Assoc 1992;201(5):777-781
- Withrow S: Mandibulectomy in the treatment of oral-cancer. J Am Anim Hosp Assoc 1983;19(3):273-286
- Lascelles BD, Thomson MJ, Dernell WS, et al: Combined dorsolateral and intraoral approach for the resection of tumors of the maxilla in the dog. J Am Anim Hosp Assoc 2003;39(3):294-305
- Farese JP, Withrow SJ: Surgical Oncology, in Withrow SJ, Vail DM, Page RL (eds): Small Animal Clinical Oncology (ed 5). St Louis, MO, Elsevier, 2013, pp 149-156
- Cray M, Selmic LE, Kindra C, et al: Analysis of risk factors associated with complications following mandibulectomy and maxillectomy in dogs. JAVMA 2021; 259(3): https://doi.org/10.2460/javma.259.3.265
- Liptak JM and Withrow SJ: Cancer of the Gastrointestinal Tract, in Withrow SJ, Vail DM, Page RL (eds.): Small Animal Clinical Oncology (ed 5). St Louis, MO, Elsevier; 2013, pp 381-395
- Beck ER, Withrow SJ, McChesney AE, et al. Canine tongue tumors: a retrospective review of 57 cases, J Am Anim Hosp Assoc 22:525, 1986.
- Sharma S, Boston SE, Skinner OT, et al. Survival time of juvenile dogs with oral squamous cell carcinoma treated with surgery alone: A Veterinary Society of Surgical Oncology retrospective study, Vet Surg 2021;50(4): 740-747
- Liptak JM, Thatcher GP, Mestrinho LA, et al. Outcomes of cats treated with maxillectomy: 60 cases. A Veterinary Society of Surgical Oncology retrospective study, VCO 2020; https://doi.org/10.1111/vco.12634
- William LE, Packer RA: Association between lymph node size and metastasis in dogs with oral malignant melanoma: 100 cases (1987-2001), J Am Vet Med Assoc 222:1234, 2003