-
Adopt
-
Veterinary Care
Services
Client Information
- What to Expect – Angell Boston
- Client Rights and Responsibilities
- Payments / Financial Assistance
- Pharmacy
- Client Policies
- Our Doctors
- Grief Support / Counseling
- Directions and Parking
- Helpful “How-to” Pet Care
Online Payments
Emergency: Boston
Emergency: Waltham
Poison Control Hotline
-
Programs & Resources
- Careers
-
Donate Now
When a dog looks up at you with puppy eyes, it can bring such a strong sense of joy — and when those same eyes become clouded with cataracts, it can be jarring.
Cataracts occur for a variety of reasons in dogs (and cats), even developing in pets who are in otherwise perfect health. Most owners will notice an obvious opaqueness appear in their dogs’ eyes and a decline in their vision. However, they might not understand why it’s happening, or how they can help.
We asked Dr. Martin Coster, DVM, MS, DACVO, a veterinary ophthalmologist at the MSPCA-Angell, to shed some light on cataracts. He shared his insight into the causes and complications associated with this common eye condition, as well as the recommended course of treatment.
Main Causes
Cataracts develop when protein fibers within the eye lens break down and clump together, causing clouding and visual impairment. Deterioration of these fibers can occur for a variety of reasons, many of which are unfortunately unavoidable.
“The majority of cataracts in dogs are hereditary/genetic, or age-related in onset, so there is very little that can be done to prevent cataract formation in these dogs,” Dr. Coster explained.
Genetic predisposition is the most prevalent cause of cataracts, with more than 90 breeds considered inherently susceptible. Among the most common breeds affected are Miniature and Standard poodles, Boston terriers, and American cocker spaniels.
As dogs grow older, they also become more prone to develop cataracts. Oxidative damage is a natural part of the aging process and it affects the entire body, including the fibers within a senior pet’s eye lens. Cataracts in dogs are distinguished from an age-related increase in density of the lens, called nuclear sclerosis, that also imparts a hazy appearance to the lens. Nuclear sclerosis affects focus ability but is not typically blinding like some cataracts.
Besides genetics and age, another major contributing cause of blinding cataracts is diabetes mellitus. Ocular conditions that can lead to cataracts include inflammation (uveitis), high eye pressure (ocular hypertension) aka glaucoma, progressive retinal atrophy, and dislocation of the eye lens (lens luxation).
Eye Exams and Early Detection

As a pet parent, you undoubtedly want to protect your pet’s eyes from cataracts. While there may be a lack of preventative measures, there are proactive ways to minimize the impact that cataracts will have on your dog’s health — starting with recognizing the early warning signs.
“Any change in color of the eye should be examined by a veterinarian,” Coster explained. “When cataracts develop rapidly (and in other instances), they can induce inflammation within the eye, which can cause redness of the white of the eye, light sensitivity, and squinting or rubbing at the eyes. Any vision change should also be assessed.”
As soon as any of these symptoms appear, a pet should have an eye exam. These signs could indicate the onset of cataracts — or a number of other eye conditions — and should be evaluated by an ophthalmologist.
For pets with a higher risk of developing cataracts (i.e., due to senior age), owners may want to consider having them examined by an eye specialist even before symptoms emerge.
“Cataracts are diagnosed by a careful and thorough eye exam, in which the ophthalmologist examines the lens/eye with magnification,” Coster said. “General practitioner veterinarians are certainly adept at diagnosing cataracts, but for early or more thorough assessment, a veterinary ophthalmologist should be consulted.”
Through these exams, veterinary ophthalmologists can ensure early detection of cataracts. Additionally, they can identify any other eye conditions that may exacerbate or accelerate the formation of cataracts. With this information, they can build a treatment plan to help manage your pet’s cataracts and promote overall eye health.
Diabetes and Cataracts

While eye exams are useful for all animals, they are crucial for pets diagnosed with diabetes. The chronic disease significantly impacts eye health, particularly with respect to cataracts.
“Approximately 80% of diabetic patients will develop significant (vision-impairing) cataracts within the first year of diagnosis of diabetes,” Dr. Coster explained.
Such a steep percentage stems from high blood sugar, which causes an increase in glucose and sorbitol (a metabolic byproduct of glucose) within a diabetic patient’s lens. To balance out this oversaturation of sugars, the body naturally draws more water into the lens, leading to swelling and, ultimately, cataracts.
In these cases, cataracts begin to form on the periphery of a pet’s lens, making them difficult to detect until they have already progressed and spread inward to cover the eye. Veterinary ophthalmologists, however, are able to spot these peripheral cataracts through examination and start therapy to alleviate secondary inflammation. For this reason, it’s recommended that dogs diagnosed with diabetes have their eyes regularly examined by a specialist, as part of their long-term care.
Although these patients are highly susceptible to cataracts, it’s possible that medication, diet, exercise and, potentially, supplementation could help delay their onset.
“It does appear that better diabetic control correlates to slower cataract formation,” Dr. Coster said.
“One study has shown that dietary supplementation with OcuGLO may slow or prevent diabetic cataract formation, and so we recommend this supplement in that patient population, where tolerated” he added.
Untreated Cataracts
Diagnosing and treating cataracts is critical — not only to improve your pet’s vision and quality of life, but also to prevent further harm.
“In the 1990s, our own Dr. Biros showed that hyper-mature cataracts (when the cataract is very ‘ripe’ and starting to shrink) have a significantly higher risk of glaucoma,” Dr. Coster explained. “Cataracts can also cause inflammation that can damage structures in the eye, leading to more complications.”
These complications include lens luxation and even retinal detachment, which may leave an animal permanently blind. Untreated cataracts also put pets at a greater risk of bodily harm, as limited or completely obscured eyesight could lead to accidents or injuries.
Treatment Options
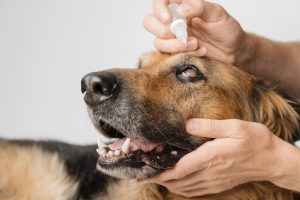
To immediately address cataracts, veterinarians may prescribe topical anti-inflammatory drops or, in more severe cases, steroids. Although these medications can temporarily alleviate some of the issues contributing to cataracts, the most effective, long-term course of treatment is surgery.
In surgery, ultrasonic waves are used to break up the cataracts before they are removed and, in most cases, an intraocular lens is implanted to aid with vision clarity. Surgical intervention is safest and most successful when the timing is right.
“Cataract surgery is preferable when the cataract is immature, as in not yet complete,” Dr. Coster said, referring to the stage when cataracts take up 10-90+% of the eye lens.
“I do talk about a ‘time window of opportunity,’” he continued. “We do not want to perform cataract surgery too early, as you risk blinding a healthy eye, but over time, the lens will get denser and harder to remove.”
Surgical outcomes are generally highly successful. 85-90% of patients experience long-term vision restoration, but blinding complications such as glaucoma or retinal detachment can occur.
Surgery Considerations
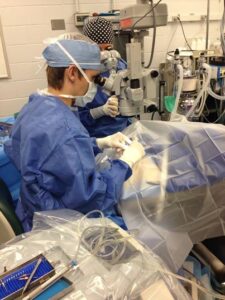
As with any procedure, there are many factors to consider when determining whether a patient is a good candidate for cataract surgery.
For instance, a pet must have a healthy retina to be eligible for surgery. Prior to the procedure, a veterinary ophthalmologist will thoroughly examine the retina through an electroretinogram (ERG) and ocular ultrasonography, confirming functional and structural stability.
Veterinarians will also assess any potential anesthetic risks associated with each case. Because cataracts are prevalent among senior dogs, age can impact whether or not anesthesia — and therefore, surgery — will be a viable option.
“In general, I have hesitancy with any patient over 13 years of age, but every patient is unique and should be evaluated and treated as such,” Dr. Coster said.
Finally, the last consideration is cost. Cataract surgery is an investment, but, if it’s financially feasible, it’s one worth making.
“Cost implications are often a driving factor in the decision to perform cataract surgery, since we rely on state-of-the-art equipment that is also used in human surgery, and this comes with a cost,” Coster explained.
“That said, we have successfully operated on patients years after their eyes have been blinded from cataracts,” he added, citing an early-career success with Bobo, a 12-year-old Chinese Crested who was able to see for the first time in two years, all thanks to surgery.




